If your jaw hurts, clicks, feels swollen near the ear, or suddenly starts catching when you chew, you do not want to wait until someone can finally “see arthritis” before taking it seriously. In my twenty years treating TMJ patients, the best outcomes almost always happen when we address inflammation early—while the joint is irritated, overloaded, and biologically active, not months later after the cartilage has taken a beating. That is why the newest treatment for TMJ is not really about chasing one trendy gadget. It is about recognizing the inflammatory phase early and treating it before the joint slides into a harder, slower-to-reverse pattern. TMJ symptoms like painful clicking, locking, neck pain, dizziness, and bite changes are all signs that the system is under stress, even if the damage is not yet dramatic on imaging.
The real early problem is often inflammation, not “just tension.”
Patients are often told their pain is stress, clenching, or “just muscle.” Sometimes that is partly true. But the joint itself is a synovial joint, and synovial joints can become inflamed before they become visibly degenerative. In painful TMJ disorders, inflammatory mediators such as TNF and matrix-degrading enzymes are implicated in pain, tissue irritation, and matrix degradation. In plain language, that means a jaw can be chemically inflamed before cartilage breakdown becomes obvious. That window matters. It is the point where smart intervention can calm the biology, reduce overload, and protect the joint from drifting into more persistent degeneration.
I recently treated a patient in her forties who had classic early joint inflammation: ear pressure, pain with chewing, one-sided clicking, morning stiffness, and headaches that wrapped into the temple. She had already been told to “watch it” because her symptoms were not severe enough for surgery and not dramatic enough on imaging. That advice cost her months. By the time she came in, the jaw muscles were guarding, the neck was tight, and the joint was flaring every time she ate anything firmer than eggs. This is what I want patients to understand: early inflammation is not harmless simply because it is early.
Why most people miss the window for TMJ pain relief
The first stage is usually subtle. You feel soreness after chewing. Your jaw opens a little crooked. You wake up stiff. You feel fullness in the ear. Then the painful clicking starts, or your mouth no longer opens as smoothly as it used to. Many patients ignore those signs because they are waiting for a dramatic lock or unbearable pain before they act. The problem is that the joint and the surrounding muscles adapt in the wrong direction. Once that guarding pattern settles in, getting lasting TMJ pain relief becomes more complicated. NIDCR lists pain in the chewing muscles or jaw joint, pain that spreads to the face or neck, jaw stiffness, locking, painful clicking, and changes in the way the teeth fit together among the key symptoms that may signal TMD.
What does not work consistently? Overstretching an inflamed joint, wearing a random over-the-counter mouth guard, hoping for the best, and grinding the bite down. Chasing permanent dental changes before the diagnosis is clear. I see patients every month who have tried three half-solutions and still cannot figure out how to help TMJ pain because nobody explained what they were actually treating. The safest starting point remains simple, conservative care: softer foods for a period, heat or cold, gentle jaw exercises, temporary anti-inflammatory support when appropriate, and stopping habits like gum chewing or constant jaw bracing. Experts also warn against treatments that permanently change the teeth, bite, or joints too early in the process.
To stop TMJ pain long-term, you have to cool the joint and correct the load causing it.
What the newest treatment for TMJ really looks like in practice
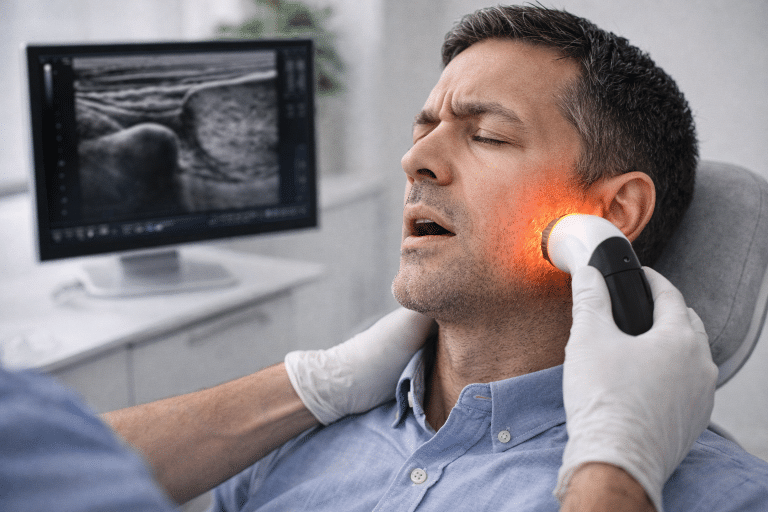
Patients often expect the newest treatment for TMJ to be one dramatic intervention. In real practice, the best newer care is layered and targeted. Low-Level Laser Therapy, also called photobiomodulation, is one of the most useful non-drug tools I use for inflamed, sensitive TMJ cases because it appears to reduce pain and improve mouth opening without mechanically aggravating the joint. When deeper tissues are involved, or the pain has become more stubborn, High-Intensity Laser Therapy can be valuable for short-term pain reduction and function. Therapeutic ultrasound still has a role in selected cases because it can calm irritated soft tissues and improve tissue extensibility. However, recent studies suggest that PBM may outperform ultrasound in achieving faster pain reduction and mouth opening. For chronic myofascial overload around the joint, Extracorporeal Shock Wave Therapy can also be helpful in carefully selected patients, as it stimulates healing and helps reset persistently dysfunctional tissue.
When inflammation is clearly intra-articular and not settling, I start thinking more precisely. Platelet-Rich Plasma, or PRP, is one of the most promising minimally invasive options in current TMJ care. Why? Platelets carry growth factors that may help modulate inflammation and improve joint function. Recent systematic reviews suggest PRP may be effective and safe for improving pain and mandibular function in temporomandibular joint disorders. In selected inflammatory or early degenerative cases, especially before more serious cartilage wear sets in, that matters. It gives us a chance to treat the biology, not just numb the pain.
Regenerative medicine helps most when it is matched to the diagnosis.
PRP is not the only regenerative tool worth discussing. Prolotherapy has gained attention for its ability to stimulate fibroblast activity, collagen synthesis, and ligamentous stabilization. In plain terms, it may help when the joint is not only inflamed but also mechanically under-supported. I consider it when ligament laxity, recurrent strain, or persistent instability are part of the picture. It is not something I recommend casually, and it is certainly not a first step for every patient, but in the right case, it can be useful.
Patients also ask me about stem cell applications because they hear them described as the future of joint repair. There is legitimate scientific interest there. But the evidence for TMJ stem cell treatment is still largely emerging and heavily preclinical, which means I discuss it honestly: promising, yes; routine front-line care, no. That distinction matters. A good physician does not sell hope by overstating the data. A good physician protects you from that.
A custom orthotic device can also be part of the plan, but only when prescribed for a specific reason. A splint should unload the joint or reduce muscle overactivity, not become a generic reflex. Used thoughtfully, it can support healing. Used unthinkingly, it can distract from the real problem. The same goes for arthrocentesis. In selected patients with clear joint inflammation, pain, and reduced range of motion that do not improve sufficiently with conservative care, early arthrocentesis can help by releasing adhesions and washing inflammatory mediators from the synovial space. That is why I do not tell patients to “just live with it” for six months when the joint is obviously not settling down.
Why therapy for TMJ pain must include muscles, posture, and sleep habits
This is where long-term success is either built or lost. The joint may be inflamed, but the neck, chewing muscles, tongue posture, and sleeping position determine whether that inflammation keeps coming back. Myofascial release techniques reduce the pull through the jaw, temples, neck, and upper chest. Trigger point therapy helps when pain radiates into the ear, cheek, or teeth from overactive muscles. Neuromuscular re-education teaches the jaw to open and close without the same crooked, defensive pattern. Targeted therapeutic exercises help restore control, not just flexibility. Recent systematic review data suggest that neck-and-jaw exercises combined with manual therapy may reduce related ear symptoms and improve function, although the evidence quality still needs strengthening.
I also spend time on postural correction protocols, stress and tension management, and sleep positioning strategies because that is often the real answer to how to stop TMJ pain from returning. If you sleep face down, brace your jaw at the computer, breathe through your mouth, or hold your tongue low and your neck forward all day, the joint never really gets a chance to stay calm. Patients searching for treatment for TMJ near me, TMJ specialist Brooklyn, TMJ specialist New York, or even TMJ disorder near me should look for someone who treats the joint, muscles, and movement pattern together—not someone who reaches for one appliance and stops there.
The message I want you to leave with is simple. The newest treatment for TMJ isn’t just about newer technology. It is earlier, smarter, more biologically informed care aimed at inflammation before cartilage breaks down, and the problem becomes harder to reverse. That is where real progress happens. That is where lasting function is protected. And that is why you should not wait for your jaw to get worse before asking the right question: not just “what can numb this,” but “what is driving the inflammation, and how do we stop it now?”