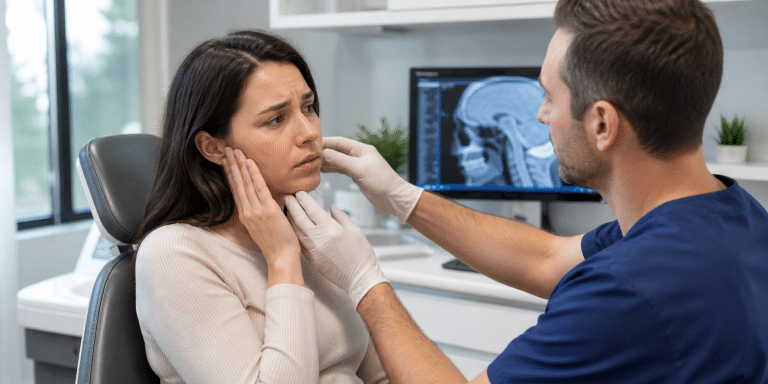
When patients search for TMJ disorder near me, they are usually not looking for theory. They are looking for relief. They want to chew without fear, wake up without jaw soreness, stop the headaches, and understand why the clicking, locking, ear pressure, or facial pain keeps returning.
In my twenty years treating TMJ patients, I have learned that many people do not fail treatment because their condition is “too severe.” They fail because the real cause was never identified. The muscles were relaxed, the pain was numbed, the night guard was handed over, but the trigger that kept the jaw from reloading was left untouched.
That overlooked cause is often instability.
Why “TMJ Disorder Near Me” Often Leads to Incomplete Answers
A patient recently came to me after trying medication, massage, a store-bought mouth guard, and months of soft foods. She had been told her TMJ pain was mostly stress. Stress was part of it, yes. But it was not the whole story.
Her jaw shifted to the right every time she opened. Her bite was uneven. Her neck muscles were pulling her head forward, which changed the resting position of her lower jaw. Her masseter and temporalis muscles were full of trigger points because they were trying to stabilize a joint that felt unsafe.
This is where many treatments miss the mark. They treat the muscle as the villain when it is often the bodyguard. Tight jaw muscles frequently protect an irritated joint, an unstable bite, a strained ligament, or a disc that is not gliding properly. Relax the muscle without correcting the reason it is guarding, and the pain returns.
That is why true TMJ pain relief starts with a better question: what is the jaw protecting against?
The Overlooked Cause: A Jaw That Keeps Guarding
The temporomandibular joint is not a simple hinge. It is a precision joint guided by muscles, ligaments, cartilage, disc movement, teeth, posture, breathing, and the nervous system. When any part of that system becomes unstable, the jaw adapts.
At first, the adaptation may feel minor. A little clicking. Some morning tightness. A headache after chewing. Then the protective pattern deepens. The muscles stay contracted longer. The joint becomes more irritated. The bite feels “off.” The patient starts chewing on one side. Sleep becomes less restorative because clenching increases at night.
So why do most treatments fail? Because they focus on calming the alarm instead of removing the threat.
If the bite is unstable, a generic mouth guard may protect the teeth but still allow the joint to compress. If the neck posture is driving the jaw backward, massage alone will not hold. If the ligaments are lax, the joint may continue to move poorly, no matter how many times the muscles are released. If deep inflammation is present, exercises may flare the patient unless the tissue is first calmed.
This is why I do not ask only, “Where does it hurt?” I ask, “What keeps making it hurt again?”
Stop Chasing Symptoms and Find the Trigger That Reloads the Jaw
The shift from temporary treatment to lasting improvement happens when we identify the reloading trigger. For one patient, that may be nighttime clenching. For another, it may be poor jaw tracking, forward head posture, disc irritation, ligament instability, or deep myofascial restriction.
This is also where a skilled examination matters. If you are searching for a TMJ specialist in Brooklyn or New York, do not choose someone who only looks at the teeth or only presses on the painful muscle. The exam should include jaw range of motion, deviation patterns, joint sounds, bite loading, cervical posture, muscle referral patterns, sleep habits, stress response, and chewing mechanics.
Once we understand the trigger, therapy for TMJ pain becomes specific. Not random. Not generic. Specific.
How Therapy Retrains the Jaw Instead of Just Relaxing It
Manual therapy is often the first doorway into relief because tight tissues must be persuaded, not forced. Myofascial release techniques help restore glide between restricted tissue layers around the jaw, temples, neck, and shoulders. Trigger point therapy can reduce referred pain into the ear, cheek, teeth, and forehead.
But release alone is not enough. The jaw must learn a safer pattern.
Neuromuscular re-education teaches the muscles to coordinate again. Many TMJ patients open their mouth by shifting, bracing, or compressing one side of the joint. They do not even realize it. Targeted therapeutic exercises retrain controlled opening, relaxed resting position, tongue posture, and symmetrical movement. These exercises are not casual stretches. They are precise corrections designed to stop the jaw from defaulting into the same painful strategy.
Custom orthotic devices also play an important role when properly designed. A splint or mouth guard should do more than separate the teeth. It should reduce joint compression, protect against destructive clenching, and support a healthier mandibular position. A poorly designed guard can make symptoms worse. A well-planned orthotic can give the joint a calmer environment while rehabilitation retrains the system.
Technology Helps When Painful Tissue Needs to Calm Down
Some patients cannot retrain effectively because the joint and surrounding tissues are too irritated. In those cases, technology-based treatments can help reduce the inflammatory load.
Low-Level Laser Therapy, also called photobiomodulation, uses light energy to support cellular repair and reduce pain signaling. High-Intensity Laser Therapy can reach deeper layers when the joint capsule, ligaments, or deeper chewing muscles are involved. Therapeutic ultrasound can help improve tissue mobility and reduce stiffness when soft tissue restriction limits normal motion.
Extracorporeal Shock Wave Therapy, or ESWT, can be useful for stubborn myofascial bands, chronic tendon irritation, and poorly vascularized tissue. It stimulates circulation and remodeling, which can help chronic pain patterns become more responsive to rehabilitation.
These are not magic tools. They work best when they are part of a larger strategy. If the tissue calms down but the bite continues to compress the joint, relapse is likely. If the tissue calms down and the jaw is retrained, the patient has a real chance to improve.
When Regenerative Medicine Belongs in TMJ Care
Some TMJ disorders involve more than muscle tension. Years of clenching, trauma, joint compression, or instability can irritate the capsule, strain ligaments, and contribute to degenerative changes.
Platelet-Rich Plasma, or PRP, uses concentrated platelets from the patient’s own blood to support healing signals in irritated tissue. Prolotherapy may help selected patients when ligament laxity allows the joint to move too much or load unevenly. Stem cell applications may be considered in carefully selected degenerative cases where evidence and clinical judgment support the discussion, but they should never be presented as guaranteed cartilage regeneration.
This is where honesty matters. Not every patient needs injections. Not every joint needs regenerative medicine. If the primary problem is a faulty movement pattern, rehabilitation is essential. If the primary problem is instability or tissue degeneration, regenerative options may become part of the plan.
The best care matches the treatment to the failing tissue.
How to Help TMJ Pain Before It Becomes Your Normal
Patients often ask me how to help TMJ pain at home. Start by reducing the daily loads that irritate the joint. Avoid gum, hard chewing, wide yawning, nail biting, and resting your chin on your hand. Keep your teeth slightly apart during the day, except when eating. Support your neck posture when working. Avoid sleeping on your stomach or pressing one side of your jaw into the pillow.
Stress and tension management also matter. That does not mean your pain is imaginary. It means your nervous system and jaw muscles are connected. When the body stays in fight-or-flight mode, clenching increases, breathing changes, and the jaw becomes more reactive. Breathing drills, relaxation training, and daytime clenching awareness can reduce the background tension that keeps the system in a state of irritation.
But self-care has limits. If pain keeps returning, if your jaw locks, if your bite changes, or if headaches and ear pressure are becoming routine, it is time to be evaluated. Searching for TMJ disorder near me is a reasonable first step. Choosing the right examination is the most important step.
TMJ pain can make you feel trapped by your own jaw. I understand how exhausting that is. But failed treatment does not mean you are out of options. It often means the true trigger has not yet been found. When the joint is unloaded, the muscles are retrained, the bite is supported, and the nervous system calms down, real recovery becomes possible. That is how to stop TMJ pain from becoming the pattern your life revolves around.