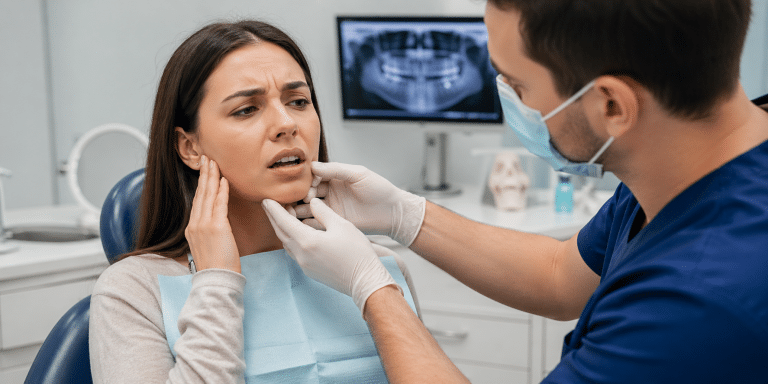
A patient from Greenpoint called my office on a Tuesday morning, voice tight with panic, and said her jaw had locked open the night before while she was eating dinner. She managed to close it after twenty minutes of gently working it with her hands, but now she could only open it about half an inch and felt pressure deep in her ear that throbbed every time she swallowed. Two days later, she added something even more concerning: her teeth no longer fit together the way they had a week earlier. She was right to be alarmed, and she was right to call quickly.
After two decades of treating jaw disorders in Brooklyn, I have learned that not every TMJ symptom carries the same weight. Most jaw clicks, mild morning soreness, and occasional headaches can be evaluated within the next several weeks. But three symptoms change that calculation entirely. When jaw locking, persistent ear pain, and sudden bite changes appear, urgent TMJ pain relief is no longer a matter of comfort. It becomes a matter of preserving the joint itself. The window for non-surgical care narrows with each week these symptoms continue, and patients who delay often pay for that delay with permanent joint damage that could have been prevented.
Why these three TMJ symptoms cannot wait
When patients ask what causes TMJ to escalate from a manageable annoyance into a true clinical emergency, the answer almost always involves a tipping point inside the joint itself. Up to a certain threshold, the joint compensates. The disc shifts slightly, the muscles tighten to protect the joint, and the patient adapts. Once the disc fully displaces, once the joint capsule becomes acutely inflamed, or once the condylar bone begins to remodel under inflammatory stress, the system is no longer compensating. It is failing. And that failure progresses unless someone intervenes.
In my practice, I see three symptoms that signal this transition more reliably than any others:
- Jaw locking, either in a closed position (cannot open fully) or an open position (cannot close)
- Persistent ear pain in the absence of an infection, especially when accompanied by jaw symptoms
- A sudden change in the way the teeth come together, even if the change feels subtle
When any of these appear, the standard advice to watch and wait or try a soft diet for a few weeks is no longer appropriate. These are signals that the joint is in active crisis, and the urgency they carry is real.
Jaw locking: closed lock, open lock, and what each one means
Locking is the most dramatic of the three. It frightens patients, and it should. There are two distinct types, each requiring a different response.
Closed lock occurs when the articular disc displaces in front of the condyle and stays there. The condyle, instead of gliding freely under the disc when the jaw opens, runs into the disc and stops. The patient typically describes a sudden inability to open the mouth beyond 25 to 30 millimeters (roughly two finger-widths), often with deviation of the jaw to the affected side. There may be a recent history of clicking that suddenly stopped, replaced by this restricted opening. That cessation of clicking is not an improvement. It is the disc becoming permanently trapped.
An open lock is the opposite of a mechanical problem. The condyle moves too far forward during opening and gets caught in front of the articular eminence, leaving the patient unable to close the jaw. This is technically a subluxation when self-reducible and a dislocation when it requires manual reduction. It often happens during a wide yawn, a dental procedure, or a large bite, and the panic it causes is significant.
Either presentation deserves immediate evaluation by a clinician who understands TMJ mechanics. Reducing a closed lock with skilled manual technique within the first two to four weeks of onset has a substantially higher success rate than waiting. The longer the disc remains displaced, the more it deforms, and the more likely surgical intervention eventually becomes necessary. For anyone searching for a TMJ disorder near me after experiencing locking, the time pressure is genuine.
Ear pain that is not actually an ear infection
Ear pain is the most commonly misdiagnosed TMJ symptom I see. Patients are often sent through multiple courses of antibiotics, ENT consultations, and imaging studies before anyone considers the temporomandibular joint. Yet the anatomy itself explains why the ear is so often involved.
The TMJ sits roughly one centimeter in front of the ear canal. The joint capsule shares innervation with structures inside the ear. The lateral pterygoid muscle attaches near tissues that influence eustachian tube function. When the joint becomes inflamed, the disc is displaced. If the retrodiscal tissue (the highly innervated area behind the disc) is irritated, or the masticatory muscles develop active trigger points, the brain interprets these signals as ear pain. The ear itself is healthy. The pain is real, but the source is the joint.
Ear pain becomes urgent when it is:
- Persistent rather than intermittent
- Accompanied by jaw symptoms such as clicking, locking, or pain on chewing
- Worse with jaw movement, talking, or eating
- Not responsive to treatment for an actual ear infection
- Accompanied by a feeling of fullness in the ear that no decongestant resolves
In these cases, the urgency stems from what the ear pain often signals: capsulitis, joint effusion, or active inflammatory damage to the joint structures. These processes are reversible early and often irreversible later. Knowing how to help TMJ pain at this stage means addressing the inflammation directly, not chasing a phantom ear infection that does not exist.
Sudden bite changes: a red flag most patients ignore
Of the three urgent symptoms, sudden bite change is the one patients most frequently dismiss. They notice that the back teeth no longer touch evenly, or that the front teeth meet differently than they did a few weeks ago, but they assume they are imagining it. They rarely imagine it.
A sudden change in occlusion (the way the teeth come together) is one of the most significant TMJ red flags in clinical practice. It indicates that something in the joint has changed enough to alter the position of the mandible itself. Possible causes include:
- Acute joint effusion, where fluid inside the joint pushes the condyle out of its normal position
- Anterior disc displacement that has shifted the condylar position
- Inflammatory arthritis affecting one or both joints
- Idiopathic condylar resorption, a serious, progressive condition in which the condylar bone breaks down, is most commonly seen in young adult women.
- Trauma-induced changes that may not have been initially apparent
Each of these requires prompt diagnostic workup, ideally including cone beam CT imaging and, in cases of suspected resorption or persistent inflammatory change, MRI. The reason this cannot wait is that condylar resorption, in particular, can progress rapidly. The bone you preserve through early intervention is bone that does not need to be reconstructed surgically later. Knowing how to stop TMJ pain in this scenario is inseparable from stopping the underlying joint deterioration that is generating the pain.
The narrowing window for non-surgical resolution
The clinical reality every TMJ patient should understand is that time matters for these three symptoms. A closed lock that has lasted two weeks reduces with manual technique in roughly seventy to eighty percent of cases. A closed lock that has lasted six months has decreased by less than 30%. A condylar resorption process caught in its early phase can often be stabilized with anti-inflammatory and regenerative care. A resorption process ignored for a year may require orthognathic surgery to restore function. Inflammatory joint changes that respond beautifully to laser, shock wave, and PRP therapy in the first three months can become structurally fixed deformities by the end of the first year. Every additional week of unaddressed locking, ear pain, or bite change moves the patient further from the non-surgical end of the treatment spectrum. Acting early is not paranoia. It is preservation.
Urgent therapy for TMJ pain that addresses the cause, not just the symptom
When a patient arrives at my office with one or more of these urgent symptoms, the treatment approach shifts from a leisurely workup to a focused, time-sensitive intervention. The goal is to stabilize the joint, reduce inflammation, restore mechanical function, and create the conditions in which the joint can heal rather than deteriorate further.
For an acute closed lock, manual reduction performed by a trained clinician is often the first intervention. The technique requires precise hand positioning and a real understanding of joint mechanics, but when successful within the early window, it can restore opening within minutes. This is followed immediately by anti-inflammatory laser therapy. Low-level laser therapy and high-intensity laser therapy reduce joint capsule inflammation at the cellular level, calm the masticatory muscles, and accelerate the recovery the joint needs to maintain its newly reduced position over the days and weeks that follow.
For acute joint inflammation and effusion, whether from disc displacement or arthritic flare, the priority is rapid reduction of inflammation. Photobiomodulation via laser therapy, combined with extracorporeal shock wave therapy (ESWT) for the surrounding muscles, addresses both the joint and the protective muscular spasm that compounds the problem. In carefully selected cases, platelet-rich plasma (PRP) therapy, injected into the joint, delivers concentrated growth factors that support the repair of damaged intra-articular tissues. For ligamentous laxity contributing to recurrent dislocation or chronic hypermobility, prolotherapy can stabilize the supporting structures over a series of treatments.
The muscular layer is never ignored in urgent cases. Active trigger points feed the protective spasm cycle that maintains joint dysfunction long after the original problem began. Myofascial release, intraoral trigger point therapy, and neuromuscular re-education all play essential roles in allowing the joint to settle into a healthier resting position. A custom orthotic, designed specifically for the patient’s mechanical pattern rather than a generic night guard, often serves as a critical bridge while the joint stabilizes.
When patients ask whether to seek a TMJ specialist in Brooklyn or in New York for these urgent presentations, the most important factor is not geography. It is whether the clinician understands the time-sensitive nature of these symptoms, has clinical experience with manual reduction techniques, has direct access to advanced imaging when needed, and can deliver coordinated drug-free, non-surgical therapy for TMJ pain across all of these layers within a single integrated treatment plan.
I have treated patients in Carroll Gardens, Prospect Heights, and Bushwick whose joints were preserved because they recognized these symptoms quickly and did not wait. I have also treated patients who waited six months, a year, or longer, and watched the treatment options narrow with each passing week. If your jaw has locked, if you are experiencing ear pain that has resisted standard ear care, or if your bite has changed in a way you cannot fully explain, please do not assume the symptom will pass on its own. Call a clinician who understands the urgency. Real TMJ pain relief is still very possible at this stage. The path is shorter, the recovery is more reliable, and the joint you save now is the joint that carries you comfortably through the next several decades of your life.
Article summary
Three TMJ symptoms signal genuine urgency and should never be ignored: jaw locking (either a closed lock from disc displacement or an open lock from subluxation), persistent ear pain in the absence of infection, and sudden changes in how the teeth fit together. Each indicates an active mechanical or inflammatory crisis inside the joint, and the window for successful non-surgical intervention narrows with every week of delay. Prompt evaluation, advanced imaging when indicated, and targeted therapy for TMJ pain, including manual reduction, low-level and high-intensity laser therapy, extracorporeal shock wave therapy, PRP, prolotherapy, myofascial work, neuromuscular re-education, and custom orthotic design can stabilize the joint and preserve long-term function when delivered early enough to matter.