If you are online searching for a TMJ specialist Brooklyn patients trust, I want to save you from one of the costliest mistakes I see in practice: booking treatment before anyone has clearly diagnosed what is actually wrong. I have treated too many patients who were given a guard, a generic exercise sheet, or a quick procedure before anyone determined whether the pain was coming from the joint, the disc, the muscles, the neck, or all of them together. That is how people lose months. Real TMJ care starts with precision. Not guesswork. And not whatever sounds newest on a website. The good news is that a careful workup usually tells us very quickly which patients need conservative care, which need imaging, and which truly need more advanced treatment.
Step 1: Ask what causes TMJ in your case, not in theory
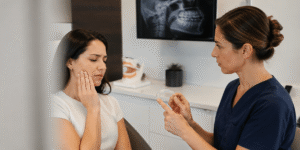
Patients often ask me what causes TMJ, as if there should be one simple answer. In real clinic life, there usually is not. NIDCR notes that injury can cause some cases. Still, for many people, the exact cause is not clear, and current research points to a mix of stress, pain processing, and other biological and behavioral factors. That is why the first diagnostic step is a detailed history, not a device. I want to know where the pain is located, when it started, whether it changes with chewing or yawning, whether it spreads to the temple or neck, whether headaches or ear symptoms are present, and whether the bite feels different. I also want to know what makes it better, what makes it worse, and whether the patient is dealing with sleep problems, other pain syndromes, or prior trauma. Until that history is clear, treatment is often just noise.
This is also the step where I rule out the many things that can masquerade as TMJ. Tooth pain, neuralgia, salivary problems, sinus pain, cervical referral, migraine, and even ear conditions can mimic jaw pain. NIDCR is explicit that pain in the mouth, jaw, or face may or may not be related to TMD, and that other conditions may need to be ruled out before the diagnosis is made. In other words, the first question is not “What treatment do I want?” The first question is “What structure is actually generating this pain?” If you skip that, even a talented clinician can end up treating the wrong target.
Step 2: A TMJ specialist Brooklyn patients trust should examine the neck, muscles, and joint together
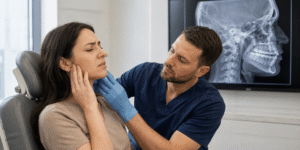
The second diagnostic step is the hands-on exam, during which weak TMJ care is identified. A real examination should include the head, face, jaw, and neck. NIDCR notes that clinicians should assess tenderness, jaw sounds, and difficulty with movement. AAFP’s review goes further, noting that common findings include tenderness of the pterygoid muscles, TMJs, temporalis muscles, the posterior cervical area, and the sternocleidomastoid. That matters because many patients think their problem is “in the joint” when the dominant pain generator is actually myofascial overload with neck involvement. I see this every week: jaw pain that worsens after laptop work, temple pressure driven by temporalis trigger points, and restricted opening caused as much by guarding as by disc mechanics.
This is also where I watch how the jaw opens. Does it deviate to one side? Is there a painful click? Is opening limited? Is there crepitus that suggests degenerative change? Does the patient brace the neck and shoulders to open the mouth? Those are not small details. They tell me whether a simple TMJ massage might help, whether the disc is likely involved, whether cervical dysfunction is feeding the problem, and whether a splint alone will almost certainly underperform. Recent evidence suggests that manual therapy and exercise targeted to the neck and jaw appear promising for reducing pain and tenderness, and that neck-and-jaw exercise with manual therapy may help with related symptoms as well. That is exactly why the neck cannot be treated like an afterthought.
Step 3: Know when imaging changes the plan
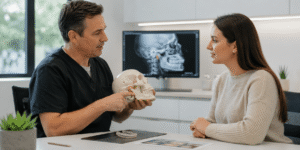
Not every TMJ patient needs imaging on day one. But some absolutely do. This is the third diagnostic step, where many rushed treatment plans fall apart. NIDCR says the clinician may suggest an X-ray, MRI, or CT. The Mayo Clinic specifies the roles more clearly: dental x-rays show the teeth and jaw, CT shows the bony structures of the joint, and MRI shows the disc and surrounding soft tissue. In practice, that means MRI is especially relevant when I suspect internal derangement, disc displacement, persistent locking, or soft-tissue pathology. In contrast, CT is more useful when I am concerned about osseous degeneration or structural change.
I recently treated a patient who had spent months being told to “stretch more” because no one had imaged a persistent locking pattern. Her issue was not a lack of effort. It was that the diagnostic sequence had been skipped. Imaging should not be ordered reflexively, but it should not be delayed when the clinical exam suggests joint pathology that would change management. That is the key point. Good imaging is not about collecting pictures. It is about preventing the wrong treatment.
The right diagnosis tells you whether you need TMJ massage, rehab, laser, or regenerative care
Once the diagnosis is clear, treatment becomes much more rational. NIDCR recommends starting with simpler, reversible care and urges caution around permanent bite changes and surgery. It also places physical therapy, manual therapy, medications, and intraoral appliances ahead of more invasive joint procedures, while listing prolotherapy and arthrocentesis in a more cautious intermediate tier. That hierarchy fits what I see in practice. The fastest way to waste a patient’s time is to use a treatment that is technically good but biologically mismatched to the diagnosis.
Why TMJ massage helps some patients – and delays others
If the case is predominantly muscular, TMJ massage can absolutely help, especially when it is part of a broader myofascial program. Myofascial release techniques can reduce abnormal tension through the masseter, temporalis, pterygoids, neck, and upper chest. Trigger point therapy can decrease referred pain into the teeth, temple, and ear. Neuromuscular re-education matters because painful jaws often move in guarded, inefficient patterns, and targeted therapeutic exercises help restore controlled opening and closing. Add postural correction protocols, stress and tension management, and sleep positioning strategies, and you finally start reducing the load that keeps reigniting the problem. But if the real issue is intra-articular inflammation, a displaced disc, or a degenerative joint surface, massage alone will feel good for a day and fail by the end of the week.
That is where newer technology-based and regenerative treatments earn their place. Low-Level Laser Therapy, or photobiomodulation, has shown benefits for pain and mandibular function across muscular and articular TMD subtypes. At the same time, a 2025 study found that PBM outperformed therapeutic ultrasound in reducing pain and improving mouth opening. High-Intensity Laser Therapy and therapeutic ultrasound can be useful adjuncts in selected cases of inflammation or soft tissue. Extracorporeal Shockwave Therapy is emerging as a potentially effective option for myogenous TMD because it may improve pain quickly and support tissue healing. For more clearly joint-driven cases, Platelet-Rich Plasma therapy appears to be a promising minimally invasive option for pain and function, and prolotherapy may have a role in selected refractory or instability-driven cases. Stem cell applications remain scientifically exciting, but the strongest evidence remains preclinical, so I discuss them as emerging rather than as routine front-line care.
Before you choose a TMJ specialist in New York or Brooklyn, make sure you know who actually performs this workup
If you are searching for a TMJ specialist in New York or a TMJ specialist in Brooklyn, office, because your jaw clicks, locks, aches, or causes pain in your temple, do not just ask who offers treatment. Ask who performs these three diagnostic steps first. Ask who examines the neck. Ask who knows when MRI changes the plan. Ask who can explain why a custom orthotic device may help one patient but not another, why manual therapy is useful in some cases, and why more advanced options should be reserved for the right diagnosis. That is the difference between a thoughtful clinician and a treatment menu.
I understand how tempting it is to book the first office that promises relief. Jaw pain is exhausting. It affects eating, sleep, mood, focus, and the simple confidence of opening your mouth without fear. But the patients who do best in the long run are usually not the ones who moved fastest into treatment. They are the ones who got the right diagnosis first. That is what I would want for my own family, and it is what I want for any patient deciding where to go next. Before you commit to treatment near you, make sure the person evaluating you is doing the work that actually deserves your trust.